Smallpox was an infectious disease caused by one of two virus variants, Variola major and Variola minor. The last naturally occurring case was diagnosed in October 1977, and the World Health Organization (WHO) certified the global eradication of the disease in 1980. The risk of death following contracting the disease was about 30%, with higher rates among babies. Some viruses exert no effect after infecting a host cell. Others, however, can be lethal. Let's take a look at six of the most dangerous viruses that.

Humans have been battling viruses since before our species had even evolved into its modern form. For some viral diseases, vaccines and antiviral drugs have allowed us to keep infections from spreading widely, and have helped sick people recover. For one disease — smallpox — we've been able to eradicate it, ridding the world of new cases.But we're a long way from winning the fight against viruses. In recent decades, several viruses have jumped from animals to humans and triggered sizable outbreaks, claiming thousands of lives.
The viral strain that drove the kills up to 90% of the people it infects, making it the.But there are other viruses out there that are equally deadly, and some that are even deadlier. Some viruses, including the around the globe, have lower fatality rates, but still pose a serious threat to public health as we don't yet have the means to combat them. Dengue(Image credit: Frederick Murphy.
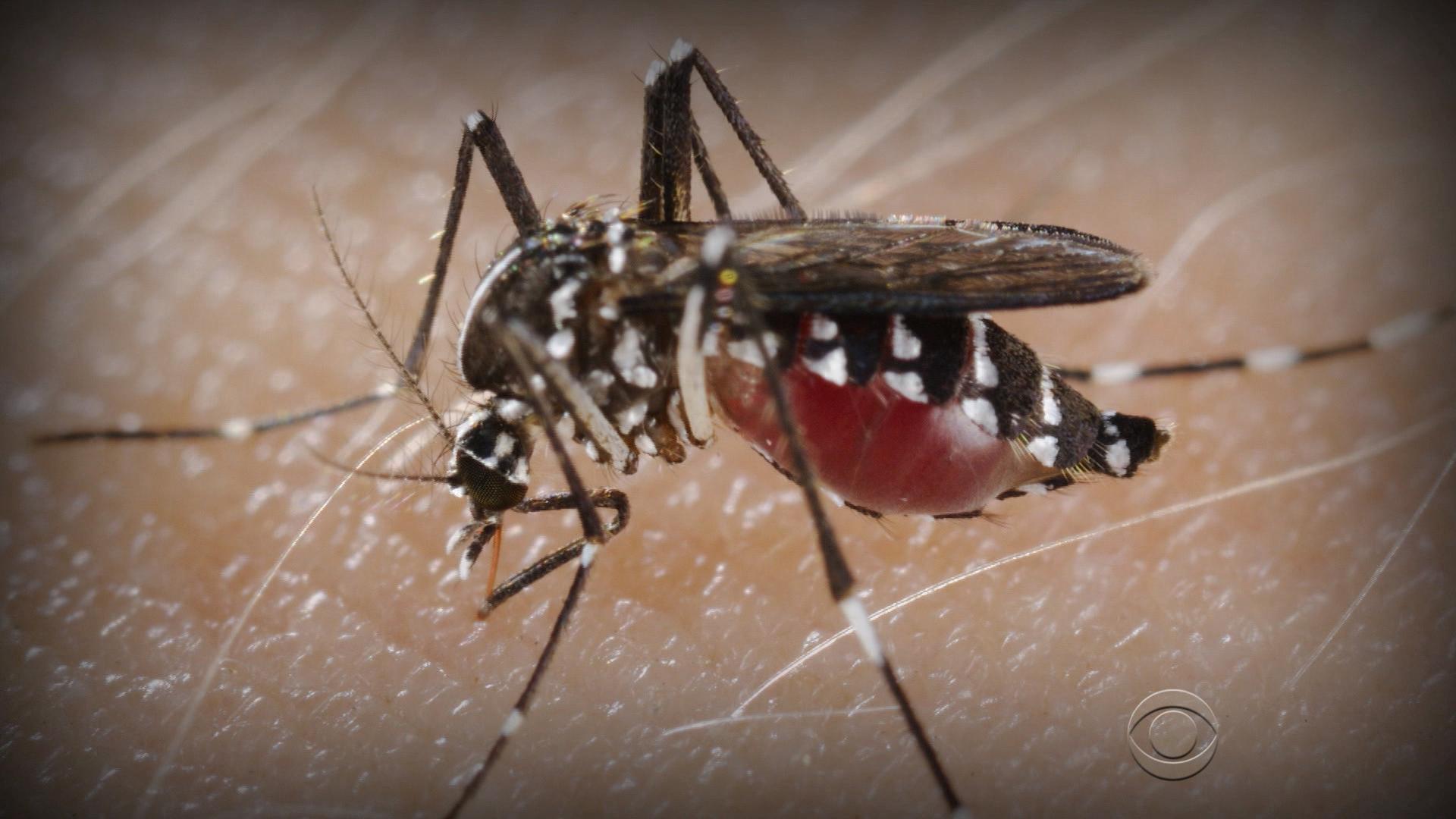
Provided by CDC/ Frederick Murphy, Cynthia Goldsmith)Dengue virus first appeared in the 1950s in the Philippines and Thailand, and has since spread throughout the tropical and subtropical regions of the globe. Up to 40% of the world's population now lives in, and the disease — with the mosquitoes that carry it — is likely to spread farther as the world warms.Dengue sickens 50 to 100 million people a year, according to WHO. Although the mortality rate for dengue fever is lower than some other viruses, at 2.5%, the virus can cause an Ebola-like disease called dengue hemorrhagic fever, and that condition has a mortality rate of 20% if left untreated. 'We really need to think more about dengue virus because it is a real threat to us,' Muhlberger said.A vaccine for Dengue was approved in 2019 by the U.S.
Food and Drug Administration for use in children 9-16 years old living in an areas where dengue is common and with a confirmed history of virus infection, according to the. In some countries, an approved vaccine is available for those 9-45 years old, but again, recipients must have contracted a confirmed case of dengue in the past. Those who have not caught the virus before could be put at risk of developing severe dengue if given the vaccine. Rotavirus(Image credit: CDC/ Dr. Palmer)Two vaccines are now available to protect children from rotavirus, the leading cause of severe diarrheal illness among babies and young children. The virus can spread rapidly, through what researchers call the fecal-oral route (meaning that small particles of feces end up being consumed).Although children in the developed world rarely die from, the disease is a killer in the developing world, where rehydration treatments are not widely available.The WHO estimates that worldwide, 453,000 children younger than age 5 died from rotavirus infection in 2008. But countries that have introduced the vaccine have reported sharp declines in rotavirus hospitalizations and deaths.
SARS-CoV(Image credit: CDC/ Dr. Fred Murphy)The virus that causes severe acute respiratory syndrome, or SARS, first appeared in 2002 in the Guangdong province of southern China, according to the. The virus likely emerged in bats, initially, then hopped into nocturnal mammals called civets before finally infecting humans. After triggering an outbreak in China, SARS spread to 26 countries around the world, infecting more than 8000 people and killing more than 770 over the course of two years.The disease causes fever, chills and body aches, and often progresses to pneumonia, a severe condition in which the lungs become inflamed and fill with pus.
SARS has an estimated mortality rate of 9.6%, and as of yet, has no approved treatment or vaccine. However, no new cases of SARS have been reported since the early 2000s, according to the. SARS-CoV-2(Image credit: NIAID-RML)belongs to the same large family of viruses as SARS-CoV, known as, and was first identified in December 2019 in the Chinese city of Wuhan. The virus likely originated in bats, like SARS-CoV, and passed through an intermediate animal before infecting people.Since its appearance, the virus has infected tens of thousands of people in China and thousands of others worldwide.
The ongoing outbreak prompted an extensive quarantine of Wuhan and nearby cities, restrictions on travel to and from affected countries and a worldwide effort to develop diagnostics, treatments and vaccines.The disease caused by SARS-CoV-2, called COVID-19, has an estimated mortality rate of about 2.3%. People who are older or have underlying health conditions seem to be most at risk of having severe disease or complications.
Common symptoms include fever, dry cough and shortness of breath, and the disease can progress to pneumonia in severe cases. MERS-CoV(Image credit: Shutterstock)The virus that causes Middle East respiratory syndrome, or MERS, sparked an outbreak in Saudi Arabia in 2012 and another in South Korea in 2015. The MERS virus belongs to the same family of viruses as SARS-CoV and SARS-CoV-2, and likely originated in bats, as well.
The disease infected camels before passing into humans and triggers fever, coughing and shortness of breath in infected people.MERS often progresses to severe pneumonia and has an estimated mortality rate between 30% and 40%, making it the most lethal of the known coronaviruses that jumped from animals to people. As with SARS-CoV and SARS-CoV-2, MERS has no approved treatments or vaccine.Follow us, &. Original article on. Meh said:The name of the virus itself, free floating without having infected anyone is SARS-CoV-2 (there's also two strains of it, an S and and L strain). When someone is infected with SARS-CoV-2, the disease is called COVID-19. One is the name of the infectious particle, the other is the name of the disease.Sorry - my mistake.
You are correct. COVID-19 is the name of the illness and not the virus itself, and the article is about the viruses. Had I read more closely, my comment would have been 'Not sure where the name SARS-CoV-2 came from. The official WHO name is 2019-nCoV.' I am new to all this. My background is engineering - not infectious organisms or diseases. Now having dug a little deeper, I see different groups seem to have different names for the same virus.
I note that the WHO says COVID-19 is different from SARS. So that has me wondering why anyone would decide to use SARS in the name if a virus that does not (according to WHO at least) cause SARS. Don't said:Sorry - my mistake. You are correct. COVID-19 is the name of the illness and not the virus itself, and the article is about the viruses. Had I read more closely, my comment would have been 'Not sure where the name SARS-CoV-2 came from. The official WHO name is 2019-nCoV.'
I am new to all this. My background is engineering - not infectious organisms or diseases. Now having dug a little deeper, I see different groups seem to have different names for the same virus. I note that the WHO says COVID-19 is different from SARS.
So that has me wondering why anyone would decide to use SARS in the name if a virus that does not (according to WHO at least) cause SARS.See here: Thus, the reference to SARS in all these virus names (combined with the use of specific prefixes, suffixes and/or genome sequence IDs in public databases) acknowledges the phylogenetic (rather than clinical disease-based) grouping of the respective virus with the prototypic virus in that species (SARS-CoV). The CSG chose the name SARS-CoV-2 based on the established practice for naming viruses in this species and the relatively distant relationship of this virus to the prototype SARS-CoV in a species tree and the distance space'. Comment on rabies fatality rate. The classic exposure /infection/terminology is difficult to employ when speaking about rabies. Although all warm-blooded animals are thought to be susceptible to rabies, there are strains of the rabies virus ( multiple bat stains ) strains are maintained in particular reservoir host(s), with some cross over especially in the US between raccoons and skunks. Although a strain can cause rabies in other species, the virus usually dies out during serial passage in species to which it is not adapted, and non-carnivores (cows, horses, deer, groundhogs, beavers ) AND CATS, like small rodents, are dead-end hosts. The CDC estimates in the US, 1 million dollars per potential life saved is spent by post-exposure prophylaxis in cases of exposure to animals other than bats, canines, fox, raccoon, skunks.
At some point, the inability to PROVE this may be trumped by statistics; when I became a veterinarian in 1975, PEP was still recommended for squirrel and gerbil bites. Hundreds of (unvaccinated) cats are infected with, and die ( or are euthanized) of rabies each year -no way every human exposure to 'the kitten in the park ' is tracked down.
Certainly, many farmers and ranchers are unknowingly exposed. Yet almost all of the 6-9 people diagnosed in the US yearly, knew they were bitten by a dog (when outside the US) or handled a bat. And there have been several incidences since 2000, where people got rabies secondary to solid organ transplants. This had been thought only a risk when transplanting 'nerve' tissue (corneas), I wonder if this reflects better and/or different immunosuppressive drugs in recipients.Species vary in susceptibility to various strains, humans are 'most' susceptible to canine rabies and, in the US, the silver-haired bat strain. This is a solitary bat with infrequent human interaction, whereas we have much more exposure to big and little brown bats and Mexican free-tailed bats.
(Only a small percentage of any of these have rabies, -it kills them too!)The virus needs to get to a nerve, so if a bite is not deep enough, or a small viral load is deposited, or the 'victim' immune system responds - an infection will never be established. If the virus is able to get to a nerve, it attempts to travel up an axon, to the brain- again, the immune system may eliminate. As rabies is a slow virus, it can self -immunize, explaining the presence of rabies neutralizing antibodies in Amazonian Indians and others who have never been vaccinated? (The reason why a mature dog is considered immunized 28 days after its first rabies vaccination, is if it has been exposed or is 'incubating' rabies virus but the virus is more than 28 days away the vaccine will prevent infection.
Although antiglobulin is given, PEP - a killed vaccine, is basically, rapid immunization. I am pulling this from memory but I believe in cases where multiple people were bitten by a rabid dog, in 15% infection was established. Once the the virus is in the brain and /or clinical signs are seen, then it is almost always, fatal. Since definitive diagnosis is made on brain biopsy, the apparent spontaneous cures or response to treatment remain unproven.Not to diminish the threat or the misery of this disease. I don't understand why the WHO estimate of deaths has been quoted as 35,000 to 55,000 for the last 40 years - while the world population went from approximately 4 billion to 8 billion, mostly in Africa and Asia where few dogs are vaccinated and most cases are seen. Admin said:Humans have been fighting viruses throughout history. Here are the 12 viruses that are the world's worst killers, based on their mortality rates, or the sheer numbers of people they have killed.
On COVID-19 origin'The virus likely originated in bats, like SARS-CoV, and passed through an intermediate animal before infecting people. '.dear admin, i don't see solid evidence and facts that this new strain of virus originated from Bats, passing thru animals, then to human. Should we sample and study the Bats or animal carcasses for more evidence? Even the latest chinese scientists from Wuhan flip to suggest that other sources is potential. Indonesia market for example has high appetite for Bats as food.It seems that humans are passing the virus to dogs and cats now.
Also, it is well known there is a P4 virus lab located nearby the Wuhan market. My question - is there any regulations that governs the building of such dangerous lab so close to the mass human neighbourhood?. Jim Thompson MD said:See here: Thus, the reference to SARS in all these virus names (combined with the use of specific prefixes, suffixes and/or genome sequence IDs in public databases) acknowledges the phylogenetic (rather than clinical disease-based) grouping of the respective virus with the prototypic virus in that species (SARS-CoV).

 RSS Feed
RSS Feed
